The maxillary sinus lift is the operation that allows you to insert dental implants where the bone is no longer enough. The success rate exceeds 97% at 5 years (meta-analysis 2021) and in the posterior area of the jaw it often represents the only path to stable and long-lasting fixed rehabilitation.
What is a maxillary sinus lift and why is it needed?
The maxillary sinus is a pneumatic cavity located above the roots of the upper posterior teeth (premolars and molars). When these teeth are lost, the underlying bone undergoes a process of progressive reabsorption: reduces both in height and thickness.
At the same time, the maxillary sinus tends to expand downwards (pneumatization). The result? Insufficient bone thickness to place a dental implant safely — in many cases less than 4-5 mm when at least 8-10 would be needed.
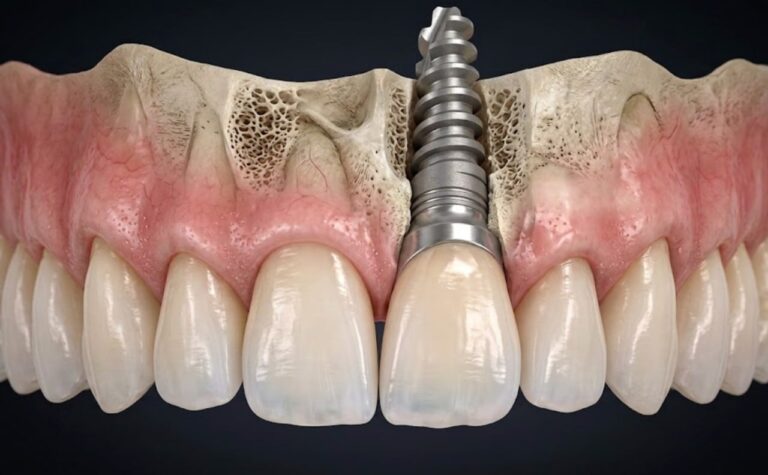
Maxillary sinus lift (in English sinus lift or sinus floor elevation) is the surgical procedure that regenerates the missing bone lifting the sinus membrane and inserting graft material into the space created. After healing, that regenerated bone becomes the solid foundation for implants.
When is maxillary sinus lift necessary?
The operation is indicated when the residual bone height in the posterior area of the upper jaw is insufficient for a standard implant. The most frequent situations are:
- Loss of upper molars or premolars occurred some time ago, with significant bone resorption
- Pneumatization of the maxillary sinus which reduced the available bone thickness
- Advanced periodontitis which compromised the bone support before extraction
- Partial or total edentulism of the upper jaw with the need for implant rehabilitation
The diagnosis is made via CBCT (Cone Beam Computed Tomography): a low-dose three-dimensional CT scan that measures the available bone with millimetric precision. In our study we use the Planmeca FACE g3, which allows ultra-low dose acquisitions with resolution up to 75 µm.
Mini raise or big rise: what's the difference?
There are two main techniques, chosen based on the residual bone height and the amount of regeneration needed.
Mini lift (crestal or transalveolar approach)
It is performed when the residual bone is between 5 and 8 mm. Access takes place through the same hole prepared for the implant: with dedicated instruments (osteotomes), the floor of the sinus is delicately raised by 2-4 mm and a small amount of biomaterial is inserted. The implant is often placed in the same session.
Advantages: shorter surgery, less post-operative edema, rapid recovery. A meta-analysis of observational studies reports implant survival rates higher than 96% at 3 years with this technique (He et al., Int J Implant Dent 2021).
Large rise (lateral approach)
It is performed when the residual bone is less than 5 mm or when it is necessary to regenerate a significant bone volume. Access takes place from the lateral wall of the maxillary sinus: a small "window" is created in the bone, the sinus membrane is raised and the cavity is filled with graft material.
A 15-year retrospective study of 472 lateral technique grafts and 757 implants reported an implant success rate of 96.8%, regardless of the type of biomaterial used (2023, J Clin Med).
Which grafting materials are used?
The choice of biomaterial is a key factor. The main options are:
- Autologous bone: taken from the same patient (chin, mandibular ramus, tuberosity). It is the biological gold standard: it contains live osteoforming cells. The disadvantage is the need for a second surgical site.
- Xenograft (heterologous bone): derived from deproteinized bovine bone (e.g. Bio-Oss®). It acts as a scaffold on which the patient's new bone grows. It is the most used in the world for breast augmentations.
- Alloplastic materials: synthetic granules (hydroxyapatite, β-tricalcium phosphate). Biocompatible and absorbable. Useful as adjuvants or alternatives.
A 2021 meta-analysis of randomized controlled trials compared augmentations with and without grafting, finding implant survival rates of 97.92% without graft and 98.73% with graft with an average follow-up of 3 years (Taha et al., Int J Oral Maxillofac Surg 2021). This means that, in expert hands, both approaches guarantee excellent results.
How is the intervention carried out, step by step?
The protocol we follow in our practice includes these phases:
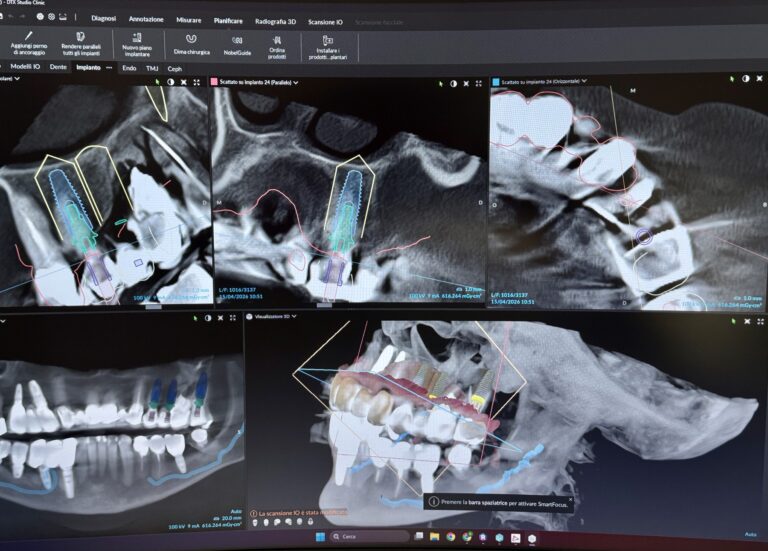
- Digital planning: CBCT acquisition with Planmeca VISO g3 for three-dimensional analysis of the anatomy of the sinus, measurement of the residual bone, identification of the bony septa and virtual planning of the operation.
- Local anesthesia: the operation is performed under local anesthesia. The patient does not feel pain during the procedure. Conscious sedation is available for more anxious patients.
- Surgical access: depending on the technique (crestal or lateral), the floor of the maxillary sinus is accessed with dedicated instruments and, when indicated, piezosurgery - which uses ultrasonic vibrations to cut the bone while protecting the surrounding soft tissues.
- Lifting of the membrane: the Schneiderian membrane (the thin mucosa that lines the sinus) is delicately lifted and detached from the bony floor. It is the most critical phase: it requires experience and precision to avoid perforations.
- Biomaterial grafting: the space created between the bone and the membrane is filled with the selected graft material, often protected by a resorbable collagen membrane.
- Implant positioning: in the mini lift, the implant is inserted in the same session. In large augmentations, we generally wait 6-8 months for the graft to mature before placing the implants.
- Suturing and follow-up: suture with absorbable threads, home antibiotic and anti-inflammatory therapy, checks at 7, 14 and 30 days.
How long does recovery take and what to expect after surgery?
The post-operative course is generally well tolerated. The first 2-3 days may present:
- Moderate edema (swelling) in the operated area
- Mild nasal bleeding on the operated side
- Sensation of pressure in the maxillary sinus
The pain is controlled with common analgesics (ibuprofen). Most patients resume daily activities after 2-3 days. The main precautions in the first 2 weeks: do not blow your nose forcefully, sneeze with your mouth open, avoid diving and flying (pressure changes).
Healing times:
- Mini increase: 3-4 months before prosthetic loading on the implant
- Large lift with simultaneous implantation: 6-8 months
- Large deferred increase (grafting → waiting → implant): 6-8 months for the graft + 3-4 months for the implant
Technology makes the difference: CBCT, microscope and piezosurgery
The precision of the intervention directly depends on the available technology. In our practice, the maxillary sinus lift uses:
- CBCT Planmeca FACE g3: three-dimensional planning with radiation dose up to 80% lower than a traditional CT scan. It allows you to visualize bone septa, anatomical variations and membrane thickness before surgery.
- Leica M525 operating microscope: magnification up to 20x for the most delicate phases, in particular the detachment of Schneider's membrane. The magnified view significantly reduces the risk of perforation.
- Piezosurgery: ultrasonic instruments that cut bone tissue with submillimeter precision without damaging the sinus membrane, vessels and adjacent nerves.
What are the risks and complications?
Like any surgical procedure, sinus lift involves risks, although the literature classifies them as infrequent and generally manageable:
- Perforation of Schneiderian membrane: is the most common complication (10-30% of cases according to the literature). If small, it is repaired with a collagen membrane during the same operation. The use of the operating microscope and piezosurgery significantly reduces its incidence.
- Post-operative sinusitis: rare (<3% of cases) if asepsis protocols and antibiotic therapy are respected.
- Bleeding: generally mild and self-limiting.
- Failure of the graft to take root: rare (< 2-3%), may require repetition of the procedure after recovery.
Maxillary sinus lift and implants: success rates
The data from the international scientific literature are reassuring. Implant survival rates after sinus lift are comparable to those of implants placed in native bone:
- 97.92-98.73% with an average follow-up of 3 years (Taha et al., Int J Oral Maxillofac Surg 2021 — meta-analysis on RCTs)
- 96.8% at 15 years old with lateral technique (2023, J Clin Med — 472 grafts, 757 implants)
- >96% at 3 years for mini ridge elevation (He et al., Int J Implant Dent 2021)
These numbers confirm that, in expert hands and with rigorous protocols, maxillary sinus lift is a reliable and predictable procedure that paves the way for long-lasting implant rehabilitations.
Frequently asked questions about maxillary sinus lift
Is the surgery painful?
No. The surgery is performed under local anesthesia and the patient does not feel pain during the procedure. Post-operatively, the discomfort can be managed with common analgesics and resolves in 2-3 days. Many patients report an easier course than expected.
How much does a maxillary sinus lift cost in Turin?
The cost varies based on the technique (mini lift vs large lift), the type of biomaterial used and the complexity of the case. It is impossible to provide a valid generic estimate: each clinical situation requires a personalized evaluation based on CBCT. For an accurate estimate, you need a first specialist visit with complete diagnostic analysis.
Can the implants be placed immediately or do we have to wait?
Depends on the residual bone. In the mini lift (residual bone 5-8 mm) the implant is almost always positioned in the same session. In large augmentations with very little residual bone, it is preferable to wait 6-8 months for the graft to mature before placing the implants, ensuring maximum predictability of the result.
Are there alternatives to maxillary sinus lift?
In some selected cases, yes: short implants (6-8 mm), inclined implants that exploit the bone available outside the sinus (All-on-4 technique), or zygomatic implants for extreme atrophy. However, sinus lift remains the gold standard when rehabilitation is desired with implants of conventional length in the posterior area, maximizing the distribution of chewing loads.
Who can perform a maxillary sinus lift?
It is an advanced surgical procedure that requires specific training in regenerative and implant surgery. Dr. Buniato trained in bone regenerative surgery at the University of Zurich and applies international protocols with precision technology (CBCT, microscope, piezosurgery) to ensure maximum safety and predictability.
Sources
- Taha et al., «Non-grafted versus grafted sinus lift procedures for implantation in the atrophic maxilla: a systematic review and meta-analysis of randomized controlled trials», Int J Oral Maxillofac Surg 2021; 50(9): 1186-1194. DOI: 10.1016/j.ijom.2021.01.015
- He et al., «The survival rate of transcrestal sinus floor elevation combined with short implants: a systematic review and meta-analysis», Int J Implant Dent 2021; 7:41. DOI: 10.1186/s40729-021-00323-0
- Tetto et al., «15-Year Retrospective Study on the Success Rate of Maxillary Sinus Augmentation and Implants», J Clin Med 2023; 12(4): 1618. DOI: 10.3390/jcm12041618
- Pjetursson et al., «A systematic review of the success of sinus floor elevation and survival of implants inserted in combination with sinus floor elevation», J Clin Periodontol 2008; 35(Suppl 8): 216-240. DOI: 10.1111/j.1600-051X.2008.01272.x
For a personalized evaluation of your case, Dr. Buniato is available for one first specialist visit with CBCT diagnostic analysis and dedicated treatment plan.